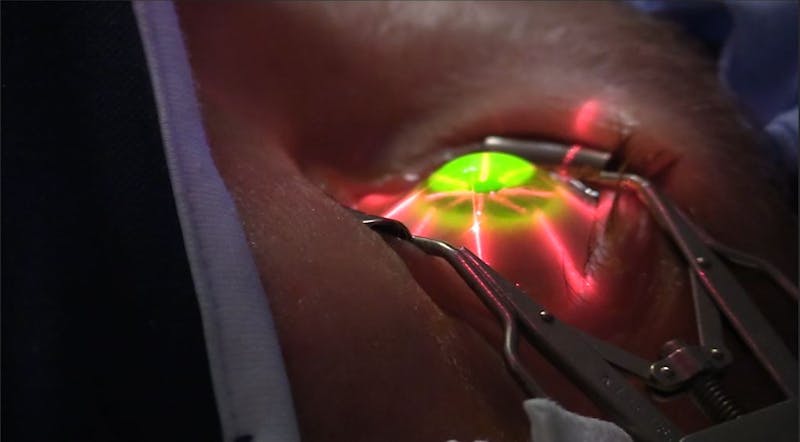
This year, Chu Vision Institute became one of the first 40 sites in the United States to join a multicenter national clinical trial evaluating the safety and efficacy of corneal cross-linking. This procedure represents a potential revolutionary new way of treating keratoconus and corneal ectasia after refractive surgery.
Characterized by thinning and steepening of the cornea, keratoconus affects approximately one out of every 1,600 people and causes irregular astigmatism, loss of best spectacle-corrected vision and myopia. Presently, the only treatment for keratoconus is the use of hard contact lenses until corneal transplant is necessary, says Y. Ralph Chu, M.D., founder and Medical Director of Chu Vision Institute and adjunct associate professor of ophthalmology at the University of Minnesota.
“Corneal transplants require a major surgery for the eye and carry potential risks of vision loss and long-term rehabilitation,” says Dr. Chu. “Cross-linking has been shown in countries outside the United States to treat patients with keratoconus and post-laser-assisted in-situ keratomileusis (LASIK) ectasia earlier in their disease processes to potentially prevent the need for corneal transplant.”
The investigational cross-linking procedure involves the removal of the corneal epithelium and administering riboflavin drops into the eye. After riboflavin administration, 365-nanome- ter ultraviolet light targets the area for approximately 30 minutes, though this period of time may vary, according to Dr. Chu.
The purpose of the procedure is to initiate linking of already- existing collagen fibrils that make up the cornea to slow the progression of keratoconus and strengthen the molecular bond between the fibrils. Dr. Chu describes the linking process as the strengthening of a suspension bridge: Ten cables provide more strength than one.
Published results demonstrate long-term improvement in patients with keratoconus who have undergone the corneal cross-linking procedure. In “Collagen Crosslinking with Riboflavin and Ultraviolet-A light in Keratoconus: Long-Term Results,” published in the Journalof Cataract and Refractive Surgery, Raiskup-Wolf, M.D., et. al. present patient data showing significant improvement in best corrected visual acuity over a three-year follow-up period.
In the multicenter trial Chu Vision Institute has joined, corneal cross-linking is also performed on patients experiencing a surgically induced form of corneal thinning called ectasia. According to Dr. Chu, patients with ectasia develop similar symptoms to keratoconus, such as astigmatism and deteriorating eyesight after LASIK surgery.
A Paradigm Shift
Chu Vision Institute presently is seeking patients ages 12 and older for the trial. According to Dr. Chu, the younger patient demographic is where the potential benefits for corneal cross- linking may be most readily seen.
“We may prevent the need for future corneal transplantation in patients who are diagnosed with keratoconus at ages 12 and 13,” says Dr. Chu. “Corneal cross-linking may potentially help them lead normal lives, which is a huge revolution for corneal procedures.”
For further information about Chu Vision Institute, visit www.ChuVision.com or call (952) 234-8295
TWIN CITIES M.D. NEWS
